Jokes about menopause used to bring a smile and a chuckle. But when it was finally my turn, it was no longer so funny. While menopause is a natural part of every woman’s life, every woman’s experience is different. Beyond the hot flashes and night sweats, a greater problem is unexpected, sometimes severe, mood changes. This article explains why you may be at a higher risk of experiencing depression and anxiety in menopause.
What Is Menopause?
First off, some basic definitions. Menopause is the natural ending of female fertility and reproductive cycles, as signified by a full year without menstrual periods. It is the counterpoint to menarche, the beginning of fertility and reproductive cycles at female puberty.
Menopause is not an event, but a progression of stages.
- The first stage is perimenopause, a time of shifting hormones leading up to the cessation of the menstrual period. Perimenopause on average is about 4 years in length, but can be as short as a few months and as long as 10 years or more.
- Menopause is the second stage, which occurs after a full year without menstrual cycles.
- The final stage, early post-menopause follows and is the five years after the cessation of menstrual cycles.
- More than five years after the last menstrual cycle is considered post-menopause.
Perimenopause starts with a shift in the normal fluctuations of the monthly hormone cycle. Estrogen and progesterone hormones begin to cycle erratically, followed by increasingly longer estrogen-less periods. These hormonal shifts can range from very gradual and almost imperceptible to sudden and chaotic.
This same shift in hormones is one of the factors that put women at a greater risk of depression and anxiety, especially in the late perimenopausal phase.
Related reading: How Depression and Anxiety Affect Relationships – All Relationships
Signs of Menopause
The shift in hormones causes many changes in your body. Other symptoms of menopause and can include: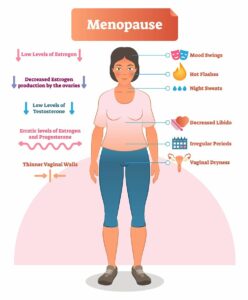
- Ceasing of menstrual periods
- Daytime hot flashes or night sweats
- Increased body fat, especially in the belly
- Less elasticity in the skin and other tissues
- Memory and concentration difficulties
- Loss of pleasure
- Mood changes and variability
- Aches, pains, and fatigue
- Sleep disturbances
- Sexual arousal disorders and/or low libido
- Digestive issues
- Frequent urination
Biological Reasons for the Greater Depression and Anxiety Risk
Most women’s experience of menopause is mainly uneventful with minimal symptoms. But for some women, it’s a different story. Women who experience multiple, severe symptoms have a lower quality of life. Especially for those with earlier experiences of anxiety and depression. The  menopausal transition is a time of biologic vulnerability for anxiety and depression relapse. This risk steadily increases during perimenopause. Studies indicate 23 percent of women will experience mood changes during this time and in post-menopause.
menopausal transition is a time of biologic vulnerability for anxiety and depression relapse. This risk steadily increases during perimenopause. Studies indicate 23 percent of women will experience mood changes during this time and in post-menopause.
Women with a history of depression are up to 5 times more likely to have a Major Depressive Disorder diagnosis during this time. Another study found that women who had low anxiety prior to peri- and postmenopause were significantly more likely to meet criteria for high anxiety when menopausal.
Shifting hormones may underlie much of the mood variations seen in menopause. The thought is erratically changing hormones affect neurotransmitters in the brain, which contributes to anxiety and depression. Other contributing factors include the effects of disrupted sleep and other menopause symptoms that erode the quality of life for some women.
Psychological Reasons for Greater Depression and Anxiety Risk
Menopause is a significant transition in a woman’s life, and a variety of emotional responses are expected. The end of fertility  causes sadness for many women and relief for others. The physical changes in the body signal aging, which causes fear, sadness, grief, resignation, anger, or other emotions depending on the individual. And, as discussed already, hormone-driven body changes can leave a woman feeling a loss of control.
causes sadness for many women and relief for others. The physical changes in the body signal aging, which causes fear, sadness, grief, resignation, anger, or other emotions depending on the individual. And, as discussed already, hormone-driven body changes can leave a woman feeling a loss of control.
For many women, significant transitions in their family life coincide with menopause. Children launch and leave home. Aging parents may need increasing care. Partners may become unwell with age-related illnesses. All these transitions can increase stress and spark anxiety or depression.
And for some women, the stress of all of this adds to an already increased risk of depression or anxiety during menopause.
Related reading: 10 Strategies for Dealing With Depression and Anxiety Without Meds
So What Can You Do?
The good news is there are a variety of things you can do to treat or at least lessen your risk of depression or anxiety in menopause.
Hormone Replacement Therapy
A recent study showed that for women without a history of depression, hormone replacement therapy (HRT) can lessen the risk of depression and anxiety in menopause. HRT minimizes many menopausal symptoms; however, HRT has risks that must be carefully considered. Always consult a physician about the appropriateness of HRT for you.
Medication
Selective Serotonin Reuptake Inhibitors (SSRIs) can be effective in combatting depression and anxiety in menopause. They are most often used in moderate to severe cases of the disorders. However, some women experience sexual side effects with these medications. Other effective medications with fewer adverse sexual side effects include bupropion (Wellbutrin) and duloxetine (Cymbalta). Some older medications, tricyclic antidepressants and monoamine oxidase (MAO) inhibitors, also can be effective. However, they carry other risks. So, make a careful evaluation with your physician.
Acupuncture
The effectiveness of acupuncture has been established for a variety of health concerns. A recent study showed that 80 percent of women in the study experienced a reduction of negative menopausal symptoms through acupuncture. This is great news for those women who do not qualify for HRT or have adverse reactions to medications. Reducing negative symptoms of menopause reduces stress, which in turn reduces the risk for depression or anxiety in menopause.
Good Health Habits
Lifestyle changes can make a significant difference in both decreasing your risk of developing anxiety or depression in menopause and diminishing their intensity, if you are experiencing them.
- Exercise – Interestingly, exercise is just as effective as antidepressants in many cases of mild depression with long-lasting results. Exercise can help you better cope with stress and may improve sleep, as well. Yoga, walking, and swimming are all gentle exercises that can make a difference. Running and other higher intensity exercises can help burn off anxiety energy.
- Reducing Caffeine and Alcohol – Caffeine, a stimulant, flares your symptoms if you’re struggling with anxiety. Alcohol, a depressant, exacerbates your depression. Reducing or avoiding your intake of caffeine and alcohol can make a real difference in your experience of anxiety or depression during menopause.
- Sleep Hygiene – Set the conditions for good sleep by eliminating all sources of light in your room, having a routine to go to bed, keeping the room below 67 degrees, and more. See this article from the National Sleep Foundation for more ideas. Sleep journals can be useful for writing down all the thoughts, keeping you up or waking you up. Seeking a therapist trained in CBT-I may also be useful.
- Self-Care – Reduce stress by using self-care techniques. This might include developing a meditation practice, regularly engaging in a hobby like gardening, getting a massage or other bodywork, and even something simple like a daily time for a cup of tea and reading. Some physicians even are prescribing time in nature to combat anxiety and other disorders. Consider a daily dose of “nature” to decrease your risk of depression and anxiety in menopause.
Counseling
If anxiety and depression are getting the best of you during menopause, counseling could be beneficial. Counselors use a variety of effective therapies for depression and anxiety, and these therapies also work during menopause. In addition to individual counseling, therapy support groups can be helpful during this time to get you back on track. If you’re in the Chicago area and think counseling would be helpful to resolve your anxiety or depression, contact us today. We have therapists in our Glen Ellyn and Jefferson Park offices ready to help.
Rhonda Kelloway, LCSW, SEP




